
The rationale for the surgical treatment of obesity has been based on three fundamental goals: (1) reducing caloric absorption by bypassing portions of the stomach and small bowel; (2) reducing gastric capacity via banding, stapling, or transection; or (3) performing operations that induce malabsorption and restrict food intake. The mechanisms of action of many of the bariatric surgical procedures may involve more than rerouting or restriction of food intake, and include alterations of metabolic pathways and other signaling processes that may modulate appetite and dietary intake.
Although the mechanisms of action of the various operations that are used to treat morbid obesity are the subject of ongoing research and are being refined, a useful paradigm is to categorize bariatric procedures as restrictive, malabsorptive, or a combination of both. The so-called restrictive procedures can certainly limit the amount of some foods that can be ingested and can induce a sense of fullness. Malabsorptive procedures alter normal nutrient digestion and absorption. Ideally, the expert bariatric surgeon should be capable of performing each operation or should be part of a team that together provides the complete range of services including the care of patients who require reoperation.
Restrictive procedures include the various gastroplasties as well as the gastric banding procedures. To perform the vertical banded gastroplasty, a small gastric pouch was created near the gastroesophageal junction with a narrowed outlet. The gastric pouch, however, originally remained in continuity with the remaining stomach. The adjustable gastric banding procedures were designed to be performed laparoscopically and position an adjustable inflatable bandlike device near the gastric cardia to limit oral intake. Of course, the adjustable gastric band can also be positioned using a traditional open approach to the abdomen.
The Roux-en-Y gastric bypass procedures were designed to combine limitation of oral intake, accomplished by restricting the size of the stomach pouch, with some malabsorption and appetite suppression by construction of the Roux limb and gastrojejunostomy. The creation of the gastrojejunostomy would inhibit intake of hyperosmolar or densely caloric foods while bypassing the distal stomach and duodenum. The reported lengths of the Roux-en-Y and afferent biliopancreatic limbs vary. Most surgeons now construct a Roux limb that is between 50 (short) and 150 cm (long) in length (usually at least 100 cm), and an afferent limb that is between 50 and 75 cm in length.
The biliopancreatic diversion disrupts intestinal absorptive capacity by short-circuiting a portion of the small intestine. However, it has not been associated with the severe complications described in patients who had jejunoileal bypasses performed. A likely explanation is that there are no defunctionalized limbs that are created.
Gastric bypass procedures and biliopancreatic diversion operations, with or without duodenal switch, account for approximately 80% of the bariatric procedures that are performed in the U.S. and Canada. Between 1998 and 2002, the number of bariatric operations performed in the U.S. increased dramatically. All of the modern procedures can be performed laparoscopically or open with acceptable mortality risks.
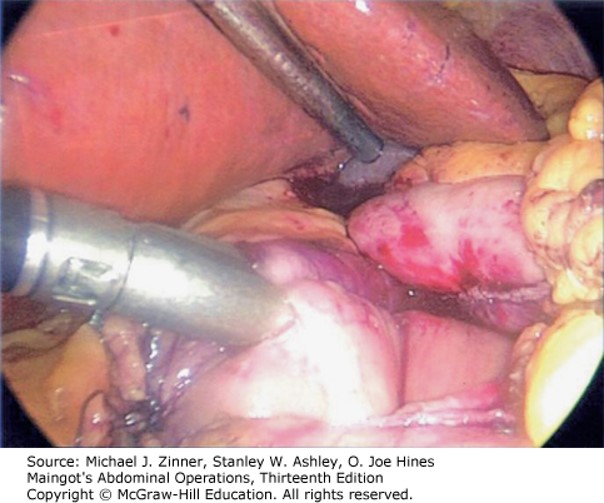 \
\Creating the gastrojejunostomy (linear stapled technique).
See a short video on Gastric Bypass from Archie MD.
Board Review Questions
1. Adjustable gastric banding (AGB) is performed around the world for treatment of clinically severe obesity. Benefits of the AGB include all of the following, except
A. easy reversibility
B. adjustable to desired weight loss
C. limited risk of malnutrition and vitamin deficiencies
D. low risk of gastrointestinal leak
E. equally successful in all patient populations
2. Following a divided Roux-en-Y GBP performed for treatment of morbid obesity, patients are prone to develop specific vitamin and mineral deficiencies. Which of the following micronutrients is least likely to be deficient in a patient who has undergone a Roux-en-Y GBP?
A. calcium
B. iron
C. vitamin K
D. folic acid
E. vitamin B-12
3. Which of the following is not a reason for the shift from vertical banded gastroplasty (VBG) to other weight loss operations?
A. mesh band erosion
B. maladaptive eating behavior
C. recurrent vomiting
D. vitamin and mineral malnutrition
E. gastrogastric fistula
Answers
1. The correct answer is E. equally successful in all patient populations
2. The correct answer is C. vitamin K
3. The correct answer is D. vitamin and mineral malnutrition

Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.