Eye Disorders Case
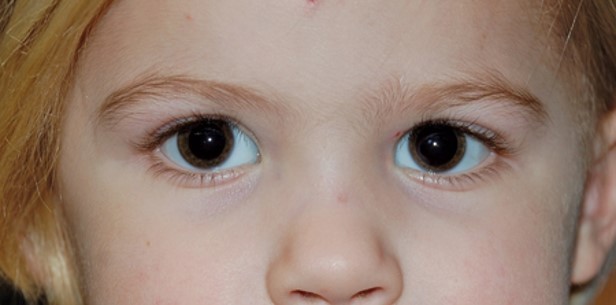
On examination, the light reflex is centered in the pupils, there is no movement on the alternate cover test, and the patient has full eye movements.
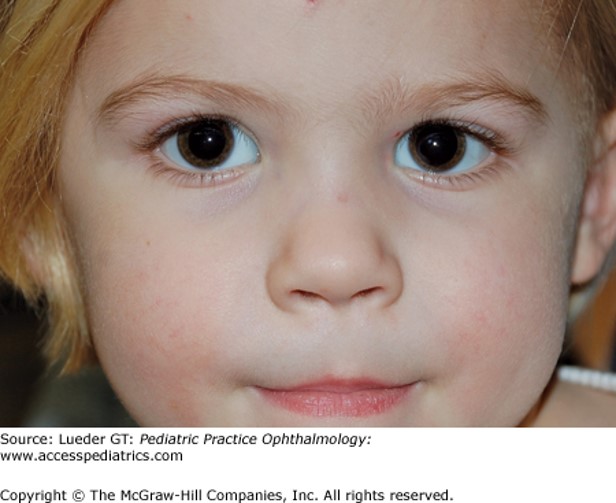
The most likely diagnosis is:
A. Fourth nerve palsy
B. Acute sixth nerve palsy
C. Intermittent exotropia
D. Accommodative esotropia
E. Pseudostrabismus
The correct answer is E.
Pseudostrabismus or pseudoesotropia is noted when the patient has broad epicanthal folds and the skin is prominent over the medial canthus, covering an increased amount of the sclera nasally, which makes the eyes appear crossed. This is also seen in children with wide nasal bridges. Alternatively, parents may believe an eye is crossed if they look at the child from the side, or take a photograph of the child from the side, and see an unequal amount of nasal sclera showing. A symmetric corneal light reflex and alternate cover test showing no movement of the eyes make true strabismus extremely unlikely. If the pediatrician is unsure of the examination findings, or if the patient has risk factors for true esotropia, such as a family history of esotropia or was born more than 2 months prematurely, the patient can be further evaluated by the pediatric ophthalmologist.
A fourth nerve palsy presents with a head tilt, or a hypertropia. This will be elicited by alternate cover testing. Both accommodative esotropia and acute sixth nerve palsy would present with true esotropia, which would be detected by a decentered corneal light reflex in 1 eye, and outward shift of the eyes on alternate cover testing, limited abduction of 1 eye, and frequently a face turn opposite the direction of abduction deficit. The most common causes of acquired sixth nerve palsy in a child are head trauma and postviral inflammation, although it can also be seen with elevated intracranial pressure, a mass lesion anywhere along the course of the sixth nerve, meningitis, intracranial hypotension, and Gradenigo syndrome (mastoiditis extending to the petrous bone). The best assessment for accommodative esotropia is with the child fixating on a small target near the examiner, such as a sticker or small toy with fine details. Accommodative esotropia is usually treated by glasses and often presents after 2 years of age. This is in contrast to infantile esotropia that is treated by surgery and is evident before 1 year of age. Intermittent exotropia can be detected when the child fixates at a distant object, and the examiner performs an alternate cover test, noting inward shift of the eyes. The history is typically of intermittent outward drift of 1 or either eye, noted primarily when the child is sick or tired, and is often more noticeable on distant gaze. (Pages 2293-2296, Section 30: Disorders of the Eyes, Part 2: Disorders of the Eye, Chapter 586)
Sources:
Question & Explanation: Cabana MD. Rudolph’s Pediatrics, 22e, Self-Assessment and Board Review New York, NY: McGraw-Hill Education; 2014.
Photo: Lueder GT. Pediatric Practice: Ophthalmology; 2011.





Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.