Pediatric Gastroenterology Case
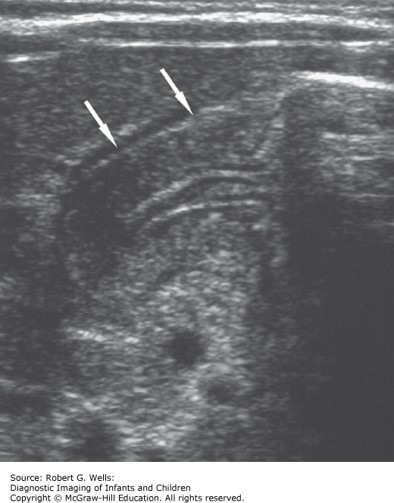
 A 6-week-old breastfed male infant presents with nonbilious, nonbloody projectile emesis with progressive worsening and recent weight loss. He has been afebrile without diarrhea. He eats voraciously then vomits, only to want to eat again.
A 6-week-old breastfed male infant presents with nonbilious, nonbloody projectile emesis with progressive worsening and recent weight loss. He has been afebrile without diarrhea. He eats voraciously then vomits, only to want to eat again.
The most likely diagnosis is:
A. Gastroesophageal reflux disease (GERD).
B. Infantile hypertrophic pyloric stenosis (IHPS).
C. Malrotation with volvulus.
D. Vascular ring
E. Formula intolerance. 
The correct answer is “B.” IHPS occurs in approximately 2 to 3.5 newborns per 1000 live births. It is more common in males than females (4:1 to 6:1) and in premature infants. It may run in families. Approximately 30% of cases occur in first-born children (approximately 1.8-fold increased risk). The etiology is unknown. Symptoms usually begin between 3 and 5 weeks of age, and very rarely occur after 12 weeks of age. Vomiting in IHPS is typically forceful and nonbilious, and tends to occur immediately after feeding. The force and timing can help to distinguish IHPS from physiologic gastroesophageal reflux, in which most episodes of vomiting are not forceful and may occur 10 minutes or more after the meal. A history of bilious vomiting does not exclude IHPS but should raise concern about more distal intestinal obstruction, such as malrotation with volvulus or Hirschsprung disease. Vascular rings typically have associated respiratory symptoms such as stridor. Option “E” is incorrect as the case clearly says the newborn is breastfed. Here’s a tip if you missed that: slow down, speedy reader! IHPS is diagnosed by ultrasound and treated surgically after rehydration and correction of electrolyte abnormalities.
Sources:
Question & Explanation: Peterson AR, Wood KE. Pediatrics Examination and Board Review. New York, NY: McGraw-Hill Education; 2017.
Photo: Chapter 35 The Stomach, Wells RG. Diagnostic Imaging of Infants and Children; 2015.






Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.