Musculoskeletal Disorders Case
A 14-month-old boy presents with refusal to bear weight on his right leg after falling off the bed.
Like
Be the first to like this
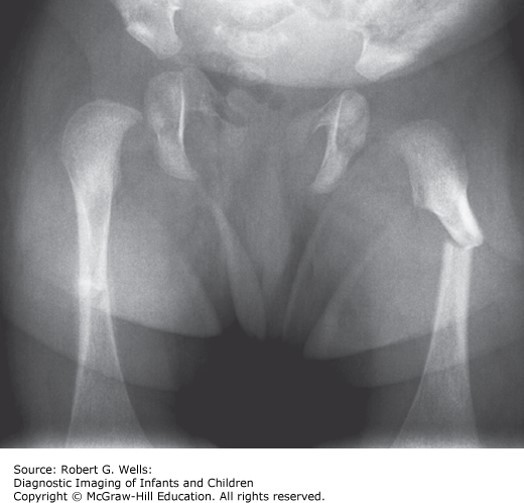
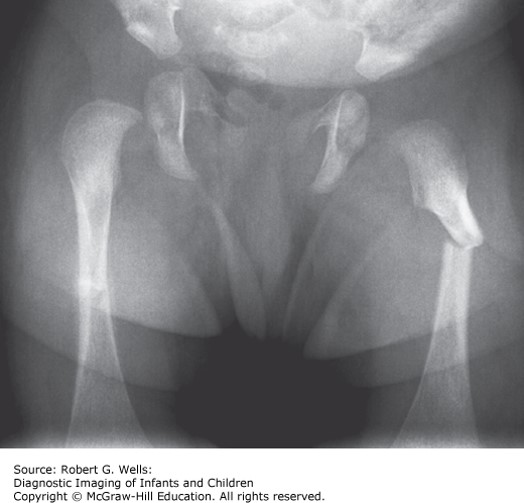
A 14-month-old boy presents with refusal to bear weight on his right leg after falling off the bed. X-rays demonstrate a midshaft femur fracture. Medical records demonstrate prior visits for a wrist fracture and a tibial fracture over the past 3 months. Physical examination reveals multiple bruises. Skeletal survey demonstrates healing right distal radius and right spiral tibial fractures, but no other healing or new fractures. Head magnetic resonance imaging (MRI) does not reveal any intracranial injury and there are no retinal hemorrhages.
Which of the following findings is least consistent with a possible diagnosis of osteogenesis imperfecta?
A. Blue sclera.
B. Dental caries.
C. Negative family history.
D. Low vitamin D level.
E. Short stature.
The correct answer is “D.” Concerns regarding osteogenesis imperfecta are frequently entertained in cases of unusual or frequent fractures and may be mistaken for nonaccidental trauma. Numerous genetic causes have been identified, most commonly in the formation of bone involving collagen (COL1A1, COL1A2, and others). Vitamin D levels are normal. Inheritance patterns of the genetic abnormalities include autosomal dominant, recessive, and X-linked forms, but current classification remains based on phenotype. Type I, or nondeforming, is the mildest, and patients typically achieve normal height. Type II is lethal in the perinatal period. Type III often presents at birth with frequent fractures and results in progressive deformity, and type IV is the moderate form. Type V involves ossification of the interosseous membrane, hypertrophic callus formation, or both. Blue sclera are common in types I and III, but individuals with type IV often have white sclera. Patients often have triangular facies and macrocephaly, and may have hearing loss. Short stature, easy bruising, and joint hypermobility may also occur. X-rays often demonstrate osteopenia or wormian bones of the skull.




Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.