Temporomandibular Joint Disorder

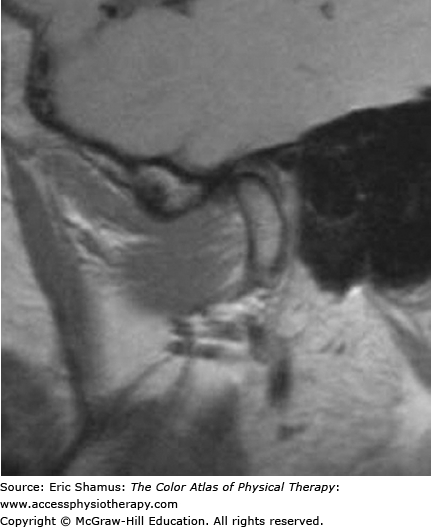

Scenario: A 32-year-old female presents at the clinic with right lateral jaw pain. The patient states she thought she had an ear infection, but the family physician stated the ear was clear. She states she has been under a lot of stress. Her husband states she grinds her teeth at night. Patient has complaints of headaches and difficulty eating apples that are uncut. Upon opening of her jaw, it is noted that the mandible deviates to the left.
Question: Besides ear infection, what are some other possible differential diagnoses that may need to be differentiated for this patient?
A. Cavity, migraines, nasal polyps
B. Sinus infection, trigeminal neuralgia, Bell’s palsy
C. Gum disease, temporal headaches, facial muscle spasm
D. Bell's palsy, facial neuralgia, migraines
Answer with rationale: b. sinus infection, trigeminal neuralgia, Bell’s Palsy. TMJ disorders and sinus infection have pain in similar areas of the head and face. They are differentiated by cause: TMJ disorders are often painful due to muscle aches, whereas sinus pain is due to congestion and swelling. TMJ disorders and trigeminal neuralgia can both cause facial pain and spasm. TMJ facial pain is often caused by diclocation of the joint disc or facial muscles, whereas pain from trigeminal neuralgia is caused by irritation of the trigeminal or 5th cranial nerve. TMJ disorders and Bell’s Palsy often have unilateral pain, discomfort and weakness in common. They are differentiated by cause: TMJ disorders are often muscular or arthrokinematic in origin, whereas Bell’s Palsy is neurological.
For more information see Chapter 111: Temporomandibular Joint Disorders in The Color Atlas of Physical Therapy




Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.