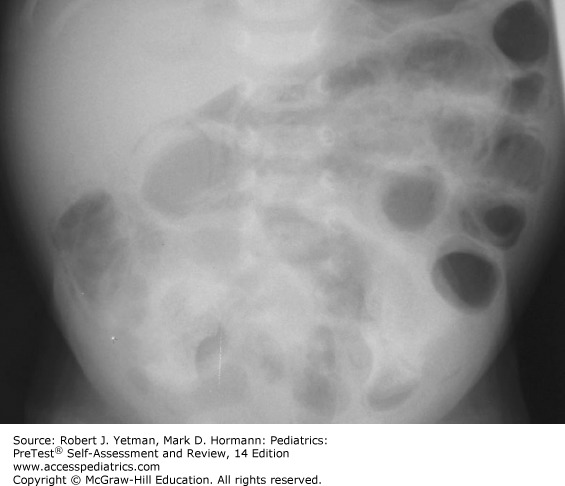
A neonatologist sees a neonate in the level 2 neonatal intensive care nursery for feeding difficulties. The 7-day-old newborn was born at 32 weeks' gestation and had been doing well on increasing nasogastric feedings of breast milk. In the previous 6 hours the nursing staff report emesis of two feedings and decreased activity. On physical examination the temperature is 36.6°C (97.9°F), heart rate is 165 beats per minute, and respiratory rate is 35 breaths per minute. The newborn is awake and appears uncomfortable. The head is normocephalic with flat fontanel. The chest is clear with good air movement and equal breath sounds. The heart has normal S1 and S2 without murmur. Abdomen is tense and distended with decreased bowel sounds. A grossly bloody stool is noted in the diaper. The plain film of his abdomen is shown. Which of the following is the most appropriate next step?
A. Obtain a surgical consultation for an emergent exploratory laparotomy.
B. Continue feeding of the newborn, as gastroenteritis is usually self-limited.
C. Culture the stool culture to identify the etiology of the bloody diarrhea and obtain an infectious disease consultation.
D. Stop feeds, begin intravenous fluids, order serial abdominal films, and initiate systemic antibiotics.
E. Remove the nasogastric tube, place a transpyloric tube, and after confirmation via radiograph of tube positioning, switch feeds from nasogastric to nasoduodenal.
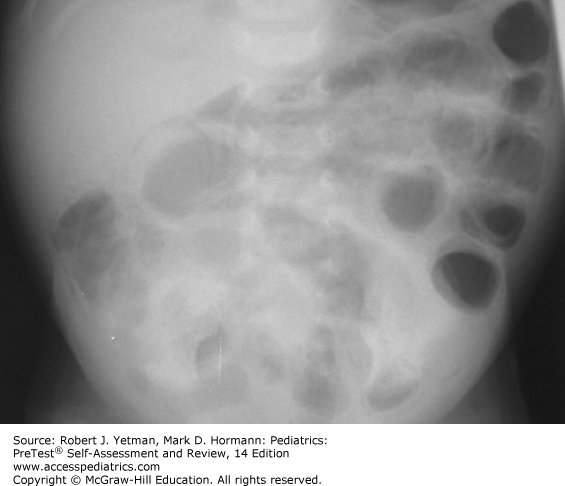
Explanation: The correct answer is D. The neonate presented in the question has the typical course of a child with necrotizing enterocolitis (NEC), a potentially life-threatening disease of the neonate. The radiograph demonstrates distended loops of bowel with air in the bowel wall (pneumatosis intestinalis). NEC is more common in premature newborns, but has been described in term neonates as well. Although several organisms have been isolated from NEC patients, no clear cause for this condition has been identified. Patients present with feeding intolerance and a distended abdomen; about a quarter have grossly bloody stool. Pneumatosis intestinalis is found on plain radiograph of the abdomen and is diagnostic for NEC in this age group. Management depends initially on the presence or absence of perforation; if no evidence of free peritoneal air is found, the newborn should be put on bowel rest with nasogastric decompression, and systemic antibiotics are initiated. Electrolytes and vital signs should be monitored closely, and serial abdominal films should be performed to evaluate for perforation. If free air is identified on plain radiographs or if the newborn clinically worsens with medical management, surgical consultation is required. An exploratory laparotomy is usually performed, and any necrotic intestinal tissue is removed. Occasionally, removal of necrotic gut will result in neonate without adequate intestinal surface area to absorb nutrition, a condition known as short bowel syndrome.





Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.