Chronic venous insufficiency, Part 1
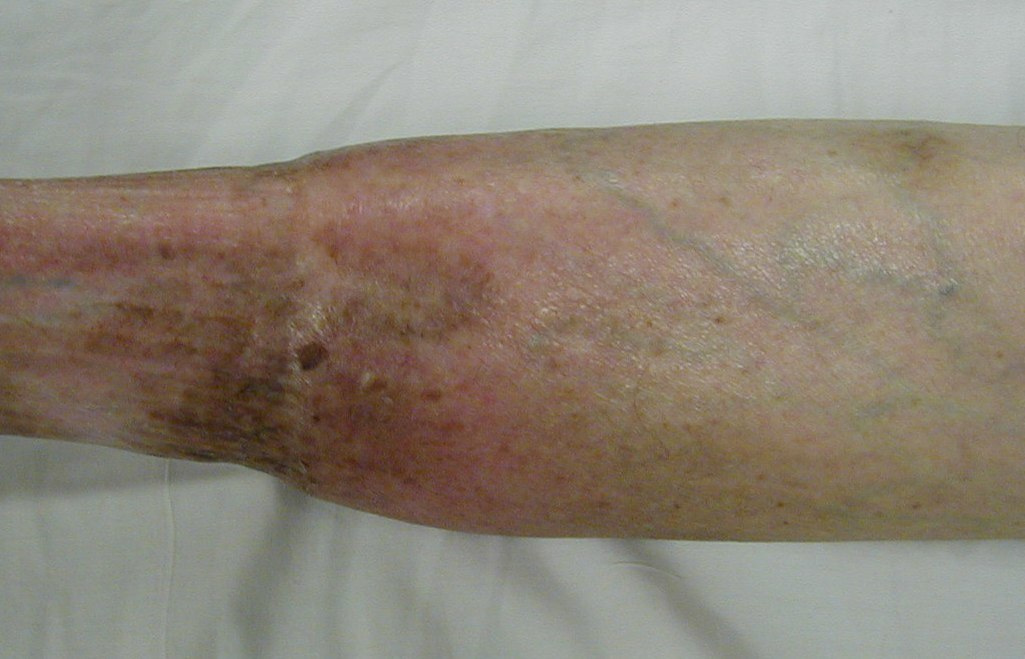
Chronic venous insufficiency
Week 7
Chronic venous insufficiency (CVI) is the primary cause of lower extremity wounds and costs an estimated $3 billion dollars in medical care annually. What are the causes, how is it diagnosed, and what is the evidence-based method of treatment? These questions will be addressed in the next few weeks.
In the photo, the most visible sign of venous disease is the tortuous, distended veins in the lower extremity. Which of the following pathologies is NOT a cause of chronic venous insufficiency?
- Venous obstruction
- Venous reflux
- Ankle immobility
- Medications
Answer D
Although certain medications can result in bilateral lower (and upper) extremity edema, venous obstruction, venous reflux due to incompetent valves, and ankle immobility with reduced function of the venous pump are the primary causes of CVI. Venous obstruction, caused by deep vein thrombosis (DVT), results in post-thrombotic syndrome (PTS) in 20-50% of the patients, and if not treated effectively, will result in skin changes and chronic venous wounds that cause further debilitation and decreased quality of life for those patients. Symptoms of PTS begin with complaints of aching, itchiness, heaviness and limb fatigue that is aggravated by prolonged standing and relieved by elevation or compression therapy. The symptoms can progress to complaints of cramping or venous claudication.
Signs of PTS begin with chronic swelling and progress to the following:
- telangiectasia (“spider veins”)
- pitting edema
- erythema, which can sometimes be an early sign of cellulitis
- hemosiderous discoloration of the lower leg due to autolysis of trapped, non-viable red blood cells in the interstitial tissue
- skin thickening, sometimes with a scaly, bark-like appearance
- secondary varicose veins (see in the photo)
- lipodermatosclerosis, or fibrosis of the subcutaneous tissue
- ulceration, usually in the gaiter area, defined as the lower one-third of the leg
The edema and discomfort can result in decreased ankle range of motion and decreased contraction of the gastro-soleus muscles during gait, which causes a pressure decrease in the venous system and thereby increases the ambulatory venous pressure (AVP). “Increased AVP leads to impaired venous return, reduced calf muscle perfusion, abnormal function of the microvasculature with increased tissue permeability, and consequently, the characteristic clinical manifestations of PTS.” (Rabinovich, 2017)
Successful prevention of PTS is imperative in order to prevent subsequent ulceration, and includes the following:
- management of the risk factors
- inadequate anticoagulation during first 3 months post DVT
- obesity (BMI > 30)
- history of ipsilateral DVT
- hormone replacement therapy (discontinue if applicable)
- elastic compression stockings
- surgical intervention for patients with extensive thrombosis
Treatment of PTS includes compression of at least 20-30 mmHg, or 30-40 mmHg if needed to control edema. Exercise has been shown to be beneficial in at least two studies, both of which recommended 6 months of leg strengthening exercises to improve calf muscle function. A good progression of exercises includes the following:
- ankle pumps
- heel/toe raises in sitting and standing
- ankle rocker board exercises
- gait training with emphasis on heel/toe sequence
- progressive walking program with incline if possible.
Further information on PTS can be found at the following sources:
Rabinovich A, Kahn ST. The postthrombotic syndrome: current evidence and future challenges. Journal of Thrombosis and Haemostasis. 2017;15:230-241. DOI: 10.1111/jth.13569.
Woelfel S, Ochoa C, Rowe VL. Vascular wounds. In Hamm R (Ed), Text and Atlas of Wound Diagnosis and Treatment: 2nd edition. New York: McGraw Hill Education. 2019, 101-143. Available at https://accessphysiotherapy.mhmedical.com/book.aspx?bookid=1334.





Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.