Remodeling or matauration of the wound
Remodeling or maturation of the wound
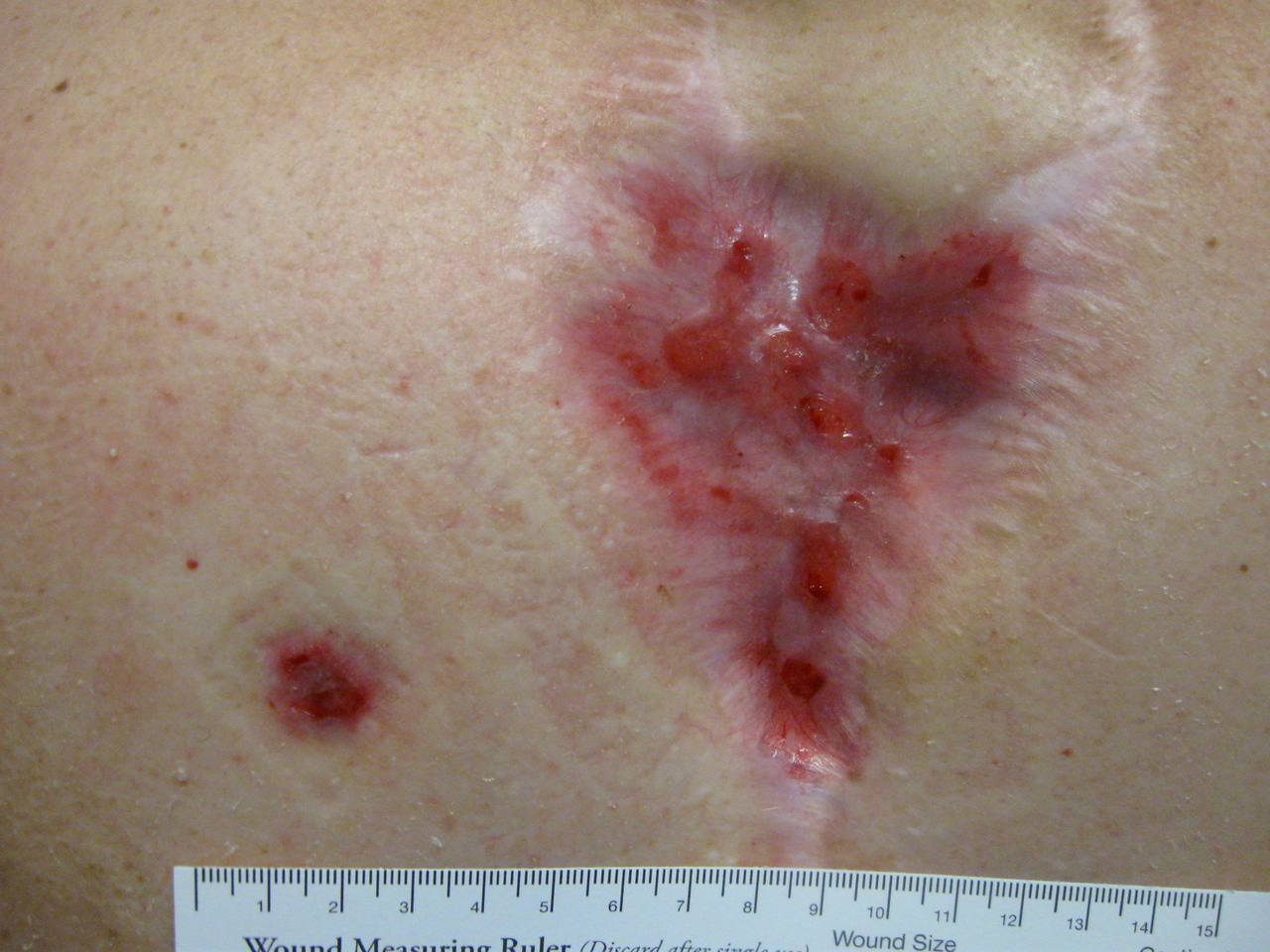
Photo 1 shows the closed lower extremity wound; however, this is not to be confused with the healed wound. Photo 2 is a dorsal thoracic post-surgical wound that is in the later stages of proliferation; however, there are some concerns regarding this wound that are discussed below.
A wound is considered fully healed when
- The surface is fully re-epithelialized.
- There is no residual pain with movement of the involved body part.
- The involved tissue has regained both functional and structural integrity.
- There is no further drainage from the wound.
Answer C
A wound is considered fully closed when it is fully epithelialized and there is no drainage; however, it is not fully healed until the tissue has regained functional and structural integrity, a process that can take from 6 month to 2 years. During this time, both cellular and acellular components are actively restoring the tissue to near-normal structure such that it will regain approximately 80% of its original tensile strength. There are multiple processes that occur during this remodeling phase of healing, including the following:
- Fibroblasts morph into myofibroblasts, cells that express α-smooth muscle actin (αSMA), a protein that is a key player in fiber contraction. The production of αSMA facilitates wound contraction, pulls the edges closer together, and decreases the area of scar tissue. Contracted edges are visible in the peripheral scarring of the thoracic wound in Photo 2.
- Epidermal cells, endothelial cells, fibroblasts and macrophages, although decreasing in number, are actively producing matrix metalloproteinases (MMPs) which degrade the excess ECM produced during the proliferative phase and thereby helps reduce scarring. The activity of MMPs is shut down by TGFß once the wound is healed. (MMP inhibitors [TIMPs] are present to balance the action of MMPs, and if there is an imbalance between the two, MMPs will degrade too many of the proteins needed for healing, and thus impair the healing process. Abnormally high levels of MMPs are known to be present in chronic wound fluid.)
- The matrix of Type III collagen that is produced during the proliferative phase is replaced by aligned Type I collagen fibers, which further promotes improved tissue function.
- Melanocytes return to the epidermal tissue, producing melanin that is subsequently stored in the keratinocytes. This process helps return the skin to its normal color and provides protection from ultraviolet rays.
- The epidermal rete pegs and dermal papillae are restored in the epidermal/dermal junction, thereby providing the strength needed to resist shear and prevent skin tears. Until this process is completed, the new skin is at risk for re-injury. If skin tearing and bleeding occur, the entire healing process has to start over.
The thoracic wound has several red flags of concern that need to be addressed: the persistent clear serous drainage from multiple areas, the thin vulnerable epithelium with spots of hyper-granulation, and the small wound that is lateral to the primary wound. This may be evidence of the MMPs/TIMPs imbalance discussed above, critical colonization of bacteria that is impeding the healing process, or protein energy malnutrition. Treatment may consist of an absorbent dressing with an antimicrobial agent and monitoring of C-reactive proteins, pre-albumin, retinal binding proteins, and zinc to determine which supplements may be indicated for this patient.
Additional information on MMPs is available at:
Caley MP, Martins VLC, O’Toole EA. Metalloproteinases and wound healing. Adv Wound Care (New Rochelle). 2015 Apr 1; 4(4): 225–234. doi: 10.1089/wound.2014.0581.
Additional information on remodeling of healing tissue is available at:
Luttrell T. Healing response in acute and chronic wounds. In Hamm R (Ed), Text and Atlas of Wound Diagnosis and Treatment, 2nd edition. New York: McGraw Hill Education. 2019;15-66. Available at https://accessphysiotherapy.mhmedical.com/book.aspx?bookid=1334.
Additional information on factors that inhibit wound healing is available at:
Hamm RL, Luttrell T. Factors that impede wound healing. In Hamm R (Ed), Text and Atlas of Wound Diagnosis and Treatment, 2nd edition. New York: McGraw Hill Education. 2019;321-346. Available at https://accessphysiotherapy.mhmedical.com/book.aspx?bookid=1334.





Create a Free MyAccess Profile
AccessMedicine Network is the place to keep up on new releases for the Access products, get short form didactic content, read up on practice impacting highlights, and watch video featuring authors of your favorite books in medicine. Create a MyAccess profile and follow our contributors to stay informed via email updates.